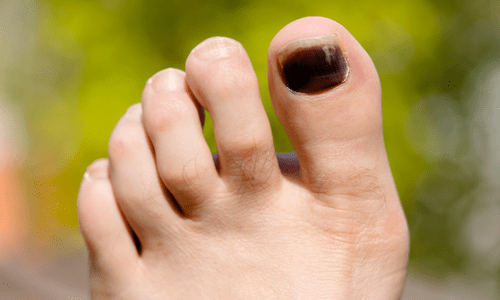
Say Goodbye to Pain: Nail Surgery is Your Path to Lasting Relief
Is a painful, recurring ingrown toenail dictating what shoes you can wear or what activities you can enjoy? You are not alone. Ingrown toenails are one of the most common foot problems we treat, and when conservative methods aren’t enough, Nail Surgery is the definitive, long-term solution. At Zest Podiatry, we are proud to offer […]
Say Goodbye to Pain: Nail Surgery is Your Path to Lasting Relief Read More »